
The Legacy
April 11, 2024
This is a guest post by Christopher Wood, Jr, son of the KCA’s late Board Chair and friend, Dr. Christopher…
Read More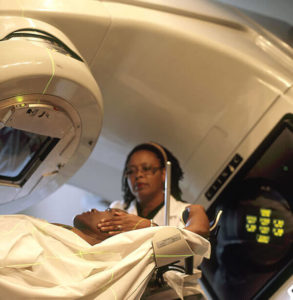
Kathryn Nelson is an RN at the Mayo Clinic in Rochester, Minnesota and a member of the KCA’s Clinical Advisory Board. In this Q & A, she talks about what radiation therapy is and when and why it might be used in the course of kidney cancer treatment.

What is radiation therapy?
Radiation therapy uses carefully targeted and regulated doses of high-energy radiation, or electromagnetic waves, to kill cancer cells. Radiation causes some cancer cells to die immediately after treatment, but most die or become incapacitated as a result of the radiation-induced damage to the cancer cell’s chromosomes and DNA. Radiation therapy can help reduce the size of some tumors. Radiation therapy can also damage normal cells in the area that is treated, though normal cells are able to repair the damage from the radiation exposure. There will be side effects from radiation, but they are usually temporary.
When and how is it used for kidney cancer?
Kidney cancers can tend to be more radioresistant, meaning they are not as sensitive to radiation therapy as other types of cancer. That makes radiation less effective as a first line of treatment for kidney cancer.
Radiation can be an option for kidney cancer patients to treat sites where the kidney cancer cells have spread or metastasized, especially in the bones and the brain. Radiation can be a way to control pain in the bones or other sites like lung metastases or spinal cord compression. Occasionally, radiation can be used to treat kidney tumors when surgery is not recommended.
How is radiation therapy delivered?
Radiation therapy can be delivered in three ways:
The type of radiation therapy that you will receive depends on what part of the body is being treated. The specific type and treatment plan that is appropriate for you will be explained by your radiation oncologist and team.
What are some of the risks, benefits, and side effects associated with radiation therapy?
Risks, benefits, and side effects of radiation therapy depend on the site being treated and the type of radiation being used. Radiation can slow down or stop tumor growth. It can decrease or alleviate pain associated with bone metastases (when cancer cells migrate to the bones).
Depending on when they occur after treatment, side effects from radiation therapy are described as acute or late onset. Acute side effects depend on the location of radiation and can include pain flares, nausea, and diarrhea. Long term side effects can include potential damage to the healthy tissues near the treatment site.
Common side effects include:
Your radiation team will explain the possible side effects and when they might develop to you and your loved ones. Don’t hesitate to ask questions.
What are some misconceptions about radiation?
Radiation does not cause you to become radioactive! When you receive radiation, it is localized to the area of treatment and not given systemically throughout the whole body like chemotherapy. Side effects are localized to the healthy tissue that is near the delivery site.
Also, radiation can be given more than once, although it cannot typically be given in the same location more than once. Radiation can be used again in areas that have not been previously treated with radiation.
What should patients and families ask about radiation oncology?
Patients and families should ask about acute or short term and long term side effects. They should alert their team about any implanted devices they have like pacemakers.
Do patients need to make any changes to a current targeted therapy or treatment plan?
Some cancer treatments may need to be stopped temporarily while undergoing radiation.
For someone who gets radiation treatment, what kind of follow up care do they need?
Follow up care is based on the site being treated and the type of radiation being utilized. Follow up could include various types of imaging – CT scans, PET scans, or an MRI, depending on what the oncology team recommends. Continue with a medical oncologist for primary care management.
Learn more about kidney cancer with the Just Diagnosed Toolkit. Download one for free in multiple languages.
1 thought on “Q & A: An Introduction to Radiation Therapy”
We appreciate you saying that your radiation oncologist and colleagues will explain the precise type and course of treatment that is right for you. My friend is battling cancer. I’ll advise her to seek out cancer-supported treatments and radiation oncologist counseling.